
What is COPD?
COPD stands for Chronic Obstructive Pulmonary Disease. It’s more than just a nagging cough or chest cold; it’s a progressive disease that affects your lungs and your ability to breathe. Learn more about COPD — its causes and risk factors, who gets it, and basic terms you should know.

Types of COPD
COPD includes chronic bronchitis and emphysema. A person can have one or both conditions.
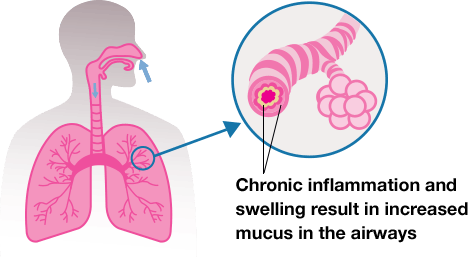
Chronic bronchitis is a condition in which the airways in your lungs (bronchial tubes) become inflamed, causing you to cough and produce more mucus than usual. The buildup of mucus and the swelling in your airways cause your airways to narrow. Bronchitis is considered chronic if you have these symptoms most days over several months, for two years in a row.
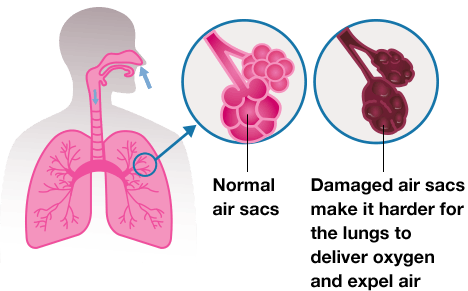
Emphysema damages the air sacs (alveoli) in the lungs. Normally, the air sacs are able to fill with air and expand like a balloon when you inhale. When you have emphysema, air sacs become less elastic, causing air to become trapped in your lungs. As a result, you are less able to exhale the normal amount of air from your lungs. This causes shortness of breath and reduces oxygen delivery from your lungs into the blood.
If you think you may have COPD, learn more about the signs and symptoms and talk to your doctor right away. While there is no cure, it's good to know there are effective treatments for COPD and things you can do to manage your symptoms and live your life.

COPD causes and risk factors
The leading cause of COPD is a history of smoking cigarettes.
In fact, smoking is linked to the vast majority of COPD cases in the US. If you smoke on a regular basis, it can inflame the linings of the airways in your lungs, leading to COPD. If you currently smoke, quitting is the best thing you can do to affect the progression of COPD and slow the decline in lung function.
In addition to smoking, other factors that can put you at risk of developing COPD are:
- Breathing in secondhand smoke
- Living in an environment that has high levels of air pollution
- Exposure to chemical fumes, dust, or pollution
- Genetics: Some people have a rare genetic condition that affects the body's ability to protect the lungs.

Who gets COPD?
COPD is more common than you may think.
Almost 16 million Americans have been diagnosed with COPD, and millions more may have the condition and are not yet diagnosed. As of 2017, COPD was the fourth leading cause of death in the US.
COPD is diagnosed more often in people over the age of 40. Although both men and women can get this disease, COPD now affects more women than men. Experts think this is because about as many women as men are smoking, and cigarette smoke may be more damaging to women’s lungs, because women typically have smaller bronchial tubes than men’s lungs. The hormone estrogen also may make women’s lungs more susceptible to tobacco smoke. In general, women tend to develop COPD earlier, even if they have had less exposure to cigarette smoke than men.

COPD definitions to know
As you read about COPD, it's helpful to understand these common terms.
Bronchodilator. A type of COPD medication that is used for relaxing the muscles around the airways in the lungs, allowing the airways to open up and expand.
Chronic bronchitis. A condition in which the airways in the lungs become inflamed, causing you to cough and produce more mucus than usual. Symptoms may be worse some days than others.
Clinical trial. A research study conducted on people to help answer specific questions about the effectiveness of new therapies, vaccines, or diagnostic procedures, or new ways of using established treatments.
Comorbidity. When two or more chronic diseases or conditions are present in your body at the same time.
COPD. Chronic Obstructive Pulmonary Disease (COPD) is a progressive lung disease that affects your ability to breathe and includes chronic bronchitis, emphysema, or both.
Emphysema. A disease that damages the air sacs in the lungs.
Exacerbation. A flare-up or worsening of COPD symptoms. There are many signs and symptoms of an exacerbation, and they can be mild, moderate, or severe.
Spirometry. A breathing test in which you blow into a special tube to measure your lung function (how well your lungs work). It shows how much air you breathe in and out of your lungs, and how quickly you can blow the air out.
Get your COPD Treatment Guide.
Answer a few questions to learn about COPD treatments that may help you or the one you care for.

